I am inclined to conclude that the studies presented here in relation to fasting and autophagy provide sufficient evidence to support a key aspect of my metabolic strategy to manage brain cancer.... and no, its not just because I am biased. ;-)
I have been experimenting with personalised fasting protocols lately, allowing for what I feel could be a theoretically viable symbiotic relationship of periodic, habitual therapeutic fasting + complimentary dose specific supplementation of fish oils + salt preparations + magnesium chloride supplementation as a specific, targeted, individualistic approach. I base this approach on my exhaustive research undertaken over the years following my diagnosis, scrutinising decades of evidence based, peer reviewed research to falsify or validate my hypotheses. I will attempt to explain why and how I believe implementation of such an approach could yield positive results for my n=1 experiment:
Numerous individuals have queried my dietary protocol, however it could reasonably be postulated, based on the evidence and underlying physiological mechanisms of this type of dietary manipulation, that the most significant benefits would likely come from calorie restriction and fasting. The metabolic state prior to commencement of a fast and personal dietary choices upon completion of such endeavours are undoubtedly of vital importance of course so as to not raise IGF-1 and upregulate mTOR during the re-feeding phase.
The gut microbiota before, during, and after fasting is another subject of great interest to me but I won't go into that because it is fairly complicated territory to cross over and I don't have time to talk about the trillions of bacteria involved despite it being critical to all aspects of health and all life on this planet as we know it... primordial poop and all that jazz.
Back to autophagy, fasting, and re-feeding....
Growth factors must be regulated via continued calorie restriction and considered selection of macro and micronutrients. In the fasted state these undesirable growth factors that act in a cascading domino fashion on reactant signalling pathways are metabolically inhibited or 'dulled' for want of a better expression (at least I tried eh? could have just said 'regulated'), so we want to continue to take advantage of this rather than cause an upsurge of insulin and contributory growth factors during the re-feeding stage. The same thing happens (the inhibition of stated growth factors) with hyperbaric oxygen therapy so it makes sense how all this fits together in powerful synergy to increase metabolic stress on tumour cells. In preparation for re-feeding I consume exogenous ketones (Ketoforce or KetoCaNa, available here http://prototypenutrition.com/ketoforce.html#!prettyPhoto to blunt the response of growth factors and to prevent over-consumption of food once I start eating again. This is to ensure that the whole practice of the fast is not counterproductive.
I believe that my restricted, dairy free ketogenic diet may effectively be mimicking (or at least I hope!) some of the favourable metabolic adaptations that come with a prolonged fasted state, with the benefit of continuous daily nourishment to maintain my current satisfactory weight. I have little stored body fat to tap in to so it would be nice to keep some functional strength and adequate bone density. On the plus side, due to the stringent approach I have adopted, my metabolic flexibility is comparable to that of a small (healthy) child.
Fasting on a ketogenic diet is something I do habitually and it can be incredibly beneficial for cancer management as I will attempt to explain. If I were a food guru I would advise against fasting because it is remarkably effective under the right circumstances and I wouldn't be able to make much money off of you with my magical foods (diminished returns you see, I can't live in a box). I may even throw the 'starvation mode' myth at you if I was feeling particularly nasty. Yes I do love 'magic mushrooms', but I also like to think I have a moral compass that guides me in the right direction when exploring these investigations and going over all the information with a fine toothed comb.
I typically aim for at least 1 day a week of no food with a controlled water intake. The benefits of intermittent fasting have been well documented both in the academic literature and to the general public over the past few years (Michael Mosley's blood sugar diet anyone?, 5:2 diet?).
For my personalised approach to periodic fasting, keeping the containment of seizure activity in mind, salts are added to my water and fluid intake is closely monitored to prevent 'breakthrough' seizures (by maintaining homeostasis of electrolytes in the brain as I expel urine throughout the fasting period). Some may also benefit from this if they ever feel light-headed during a fast but this may simply be the case if they are not metabolically adapted to utilising fats as a predominant fuel source. On a well structured ketogenic diet for cancer management this should be a seamless transition because the diet itself mimics a fasted state as mentioned previously in this post. In this state fatty acids are already an obligitory source of cellular energy production by peripheral tissues and also the brain of course.
Can we query current rationalities and approaches to nutrigenomics?
The pre-eminent curiosity that I retain regarding health practitioners is that specialists in nutrition on occasion appear to not possess the adequate level of biochemical grounding to explain the vital processes happening at the cellular level during fasting and through manipulation of eicosanoids (fatty acids), conversely from my personal experiences, experts in biochemistry don't apply their vast knowledge of these complex physiological systems to basic fundamentals of nutrition in a sensible, practical sense. In other words, the nutrition experts sometimes oversimplify very complicated metabolic processes and the biochemist could be overcomplicating his or her work that could be applied practically via simple means. This is purely based on observational, subjective personal extrapolations of course. Disclaimer, don't shoot me. ;-)
I suggest a more balanced approach where these complicated mechanisms are explained in sufficient detail and with careful cogitation, along with their appropriate practical applications. In other words why go around the moon to get to the sun even though space travel in itself is complicated. A rocket scientist has a complicated job but we have sent monkeys into space. The monkey just needs to know how to practically apply this information with enough detail. You can probably tell by now that I like my appreciably contrived analogies. With a new dawn of 'personalised medicine' approaching on the horizon however, I am encouraged by the direction in which we are heading.
Autophagy- essentially the process of 'self-eating'!... in a good way (clearing out the rubbish)
As we begin to think about autophagy in general, and the specific mechanisms of mitophagy, the genius of the human body's innate natural survival adaptations reveal themselves in quite remarkable ways. Its all very clever when we delve just a little deeper into it. If we don't feed the body it will be more efficient at doing some essential housekeeping! I feel it is appropriate to give the analogy of someone who has a messy house, cleaned once per week (typically Sunday because there are less time constraints and other responsibilities to deal with). The house can be cleaner if all resources can be employed to the task at hand with no alternative concurrent responsibilities. With respect to our physiological requirements in a fasted state, the digestive system is able to take a much needed rest from metabolising nutrients from food, focusing all of its energies on cleansing organs, doing some dusting, and clearing out the rubbish!
I have been experimenting with personalised fasting protocols lately, allowing for what I feel could be a theoretically viable symbiotic relationship of periodic, habitual therapeutic fasting + complimentary dose specific supplementation of fish oils + salt preparations + magnesium chloride supplementation as a specific, targeted, individualistic approach. I base this approach on my exhaustive research undertaken over the years following my diagnosis, scrutinising decades of evidence based, peer reviewed research to falsify or validate my hypotheses. I will attempt to explain why and how I believe implementation of such an approach could yield positive results for my n=1 experiment:
Numerous individuals have queried my dietary protocol, however it could reasonably be postulated, based on the evidence and underlying physiological mechanisms of this type of dietary manipulation, that the most significant benefits would likely come from calorie restriction and fasting. The metabolic state prior to commencement of a fast and personal dietary choices upon completion of such endeavours are undoubtedly of vital importance of course so as to not raise IGF-1 and upregulate mTOR during the re-feeding phase.
The gut microbiota before, during, and after fasting is another subject of great interest to me but I won't go into that because it is fairly complicated territory to cross over and I don't have time to talk about the trillions of bacteria involved despite it being critical to all aspects of health and all life on this planet as we know it... primordial poop and all that jazz.
Back to autophagy, fasting, and re-feeding....
Growth factors must be regulated via continued calorie restriction and considered selection of macro and micronutrients. In the fasted state these undesirable growth factors that act in a cascading domino fashion on reactant signalling pathways are metabolically inhibited or 'dulled' for want of a better expression (at least I tried eh? could have just said 'regulated'), so we want to continue to take advantage of this rather than cause an upsurge of insulin and contributory growth factors during the re-feeding stage. The same thing happens (the inhibition of stated growth factors) with hyperbaric oxygen therapy so it makes sense how all this fits together in powerful synergy to increase metabolic stress on tumour cells. In preparation for re-feeding I consume exogenous ketones (Ketoforce or KetoCaNa, available here http://prototypenutrition.com/ketoforce.html#!prettyPhoto to blunt the response of growth factors and to prevent over-consumption of food once I start eating again. This is to ensure that the whole practice of the fast is not counterproductive.
 |
| The benefits of fasting: mTor in the spotlight- IMG- http://jcs.biologists.org/content/120/3/379 |
 |
| Fasting helps to regulate cascading signalling pathways like mTor and IGF-1. Turbulence must ideally be steadied in the midst of the re-feeding phase, maintaining consistent, therapeutic blood glucose readings. IMG- http://www.anbg.gov.au/flags/semaphore.html |
Fasting on a ketogenic diet is something I do habitually and it can be incredibly beneficial for cancer management as I will attempt to explain. If I were a food guru I would advise against fasting because it is remarkably effective under the right circumstances and I wouldn't be able to make much money off of you with my magical foods (diminished returns you see, I can't live in a box). I may even throw the 'starvation mode' myth at you if I was feeling particularly nasty. Yes I do love 'magic mushrooms', but I also like to think I have a moral compass that guides me in the right direction when exploring these investigations and going over all the information with a fine toothed comb.
I typically aim for at least 1 day a week of no food with a controlled water intake. The benefits of intermittent fasting have been well documented both in the academic literature and to the general public over the past few years (Michael Mosley's blood sugar diet anyone?, 5:2 diet?).
For my personalised approach to periodic fasting, keeping the containment of seizure activity in mind, salts are added to my water and fluid intake is closely monitored to prevent 'breakthrough' seizures (by maintaining homeostasis of electrolytes in the brain as I expel urine throughout the fasting period). Some may also benefit from this if they ever feel light-headed during a fast but this may simply be the case if they are not metabolically adapted to utilising fats as a predominant fuel source. On a well structured ketogenic diet for cancer management this should be a seamless transition because the diet itself mimics a fasted state as mentioned previously in this post. In this state fatty acids are already an obligitory source of cellular energy production by peripheral tissues and also the brain of course.
 |
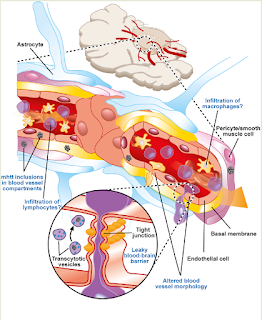
| I can have 'breakthrough' seizures if I fail to maintain desirable therapeutic ratios of electrolytes in the brain. IMG- http://www.bioquicknews.com/node/1863 |
The pre-eminent curiosity that I retain regarding health practitioners is that specialists in nutrition on occasion appear to not possess the adequate level of biochemical grounding to explain the vital processes happening at the cellular level during fasting and through manipulation of eicosanoids (fatty acids), conversely from my personal experiences, experts in biochemistry don't apply their vast knowledge of these complex physiological systems to basic fundamentals of nutrition in a sensible, practical sense. In other words, the nutrition experts sometimes oversimplify very complicated metabolic processes and the biochemist could be overcomplicating his or her work that could be applied practically via simple means. This is purely based on observational, subjective personal extrapolations of course. Disclaimer, don't shoot me. ;-)
 |
| The alimentary canal- human digestive tract. IMG- http://igbiologyy.blogspot.co.uk/2013/04/52-human-alimentary-canal.html |
 |
| Eicosanoids and cancer- could nutrition professionals benefit from a greater understanding of the numerous underlying processes of physiological processes to improve complimentary treatment protocols? IMG- http://www.nature.com/nrc/journal/v10/n3/fig_tab/nrc2809_F3.html |
 |
 |
| Because I want to break free- a significant role of mitophagy involves the removal of damaged, depolarised mitochondria. Nutrient deprivation is the key activator of autophagy. |
I found this great explanation of autophagy via Dr. Jason Fung's article on fasting and autophagy which details everything better than I can! I really admire his work. You can follow the link on the picture below to learn more.
 |
|
|
I mentioned all of this in my Youtube video. I have added it here to act as a sort of appendix:
What is clear to me is that there are several benefits to these physiological responses to fasting and calorie restriction. I wanted to show that this can be explained through the basic fundamentals of cell biology.
What is clear to me is that there are several benefits to these physiological responses to fasting and calorie restriction. I wanted to show that this can be explained through the basic fundamentals of cell biology.
In my Youtube video I mentioned expression of FGF21 and PARa during fasting in humans and other animals. Its complicated but there are numerous benefits to this in relation to fasting. The diagram may help to detail the biochemical mechanisms better than I can. Clear as mud?  |
| IMG-http://www.nature.com/nm/journal/v19/n9/fig_tab/nm.3334_F1.html |
'There are multiple interactive pathways and molecular mechanisms by which CR (calorie restriction) and IF (intermittent fasting) benefit neurons including those involving insulin-like signaling, FoxO transcription factors, sirtuins and peroxisome proliferator-activated receptors. These pathways stimulate the production of protein chaperones, neurotrophic factors and antioxidant enzymes, all of which help cells cope with stress and resist disease. A better understanding of the impact of CR and IF on the aging nervous system will likely lead to novel approaches for preventing and treating neurodegenerative disorders.' http://www.sciencedirect.com/science/article/pii/S1568163706000523
This study shows that circulating levels of FGF21 are markedly increased by fasting in humans and are part of the late stages of the body's adaptive response to starvation — a protective mechanism that evolved to aid survival in periods of famine. http://www.nature.com/nrendo/journal/v12/n1/full/nrendo.2015.202.html
The Peroxisome Proliferator Activated Receptor alpha (PPARα) is a transcription factor that plays a major role in metabolic regulation. The map puts PPARα at the center of a regulatory hub impacting fatty acid uptake, fatty acid activation, intracellular fatty acid binding, mitochondrial and peroxisomal fatty acid oxidation, ketogenesis, triglyceride turnover, lipid droplet biology, gluconeogenesis, and bile synthesis/secretion. In addition, PPARα governs the expression of several secreted proteins that exert local and endocrine
functions. http://www.sciencedirect.com/science/article/pii/S221287781400043X
functions. http://www.sciencedirect.com/science/article/pii/S221287781400043X
It all actually started for me with the Valter Longo studies for cancer management as soon as I received my diagnosis and read 'Cancer as a Metabolic Disease'. Here are some of those studies that sparked my initial enthusiasm for this approach:
Dietary restriction and cancer management
http://www.nature.com/onc/journal/v30/n30/abs/onc201191a.html
Fasting and IGF-1
http://cancerres.aacrjournals.org/content/70/4/1564.short
Fasting cycles retard growth of tumours and sensitise a range of cancer cell types to chemotherapy
http://stm.sciencemag.org/content/scitransmed/4/124/124ra27.full
Dietary restriction and cancer management
http://www.nature.com/onc/journal/v30/n30/abs/onc201191a.html
Fasting and IGF-1
http://cancerres.aacrjournals.org/content/70/4/1564.short
Fasting cycles retard growth of tumours and sensitise a range of cancer cell types to chemotherapy
http://stm.sciencemag.org/content/scitransmed/4/124/124ra27.full